AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
Back to Blog
Base metacarpal fracture12/7/2023 
4 While most patients have some degenerative changes radiographically, surprisingly there is no correlation with symptoms. Long-term functional outcome studies have shown that strength of the affected hand is decreased in all patients regardless of the type of treatment. Structurally, metacarpal bones can be divided into four parts- base, shaft. Because screw fixation is more secure, active range of motion may be initiated 5 to 10 days postoperatively. Metacarpals consist of five long bones that connect the carpals with the phalanges. Postoperatively, if pins are used, the thumb is immobilized in a thumb spica cast for 4 weeks. 3 Under direct vision, either Kirschner wires or lag screws can be inserted to hold the reduction in place. If one cannot achieve anatomical closed reduction with an intra-articular step off of not more than 2 mm, then open reduction and internal fixation should be performed. 2023 ICD-10-CM Codes S62.2: Fracture of first metacarpal bone. This wire remains in place for a period of 4 weeks, at which time the wire is removed and a rehabilitation program is started. Percutaneous Kirschner wires can be inserted through the base of the metacarpal, across the joint, and into the trapezium to hold the reduction in place. Operative treatment with closed reduction and percutaneous pinning is often attempted first. Most authors now recommend improvement of the metacarpal subluxation with percutaneous or open reduction. 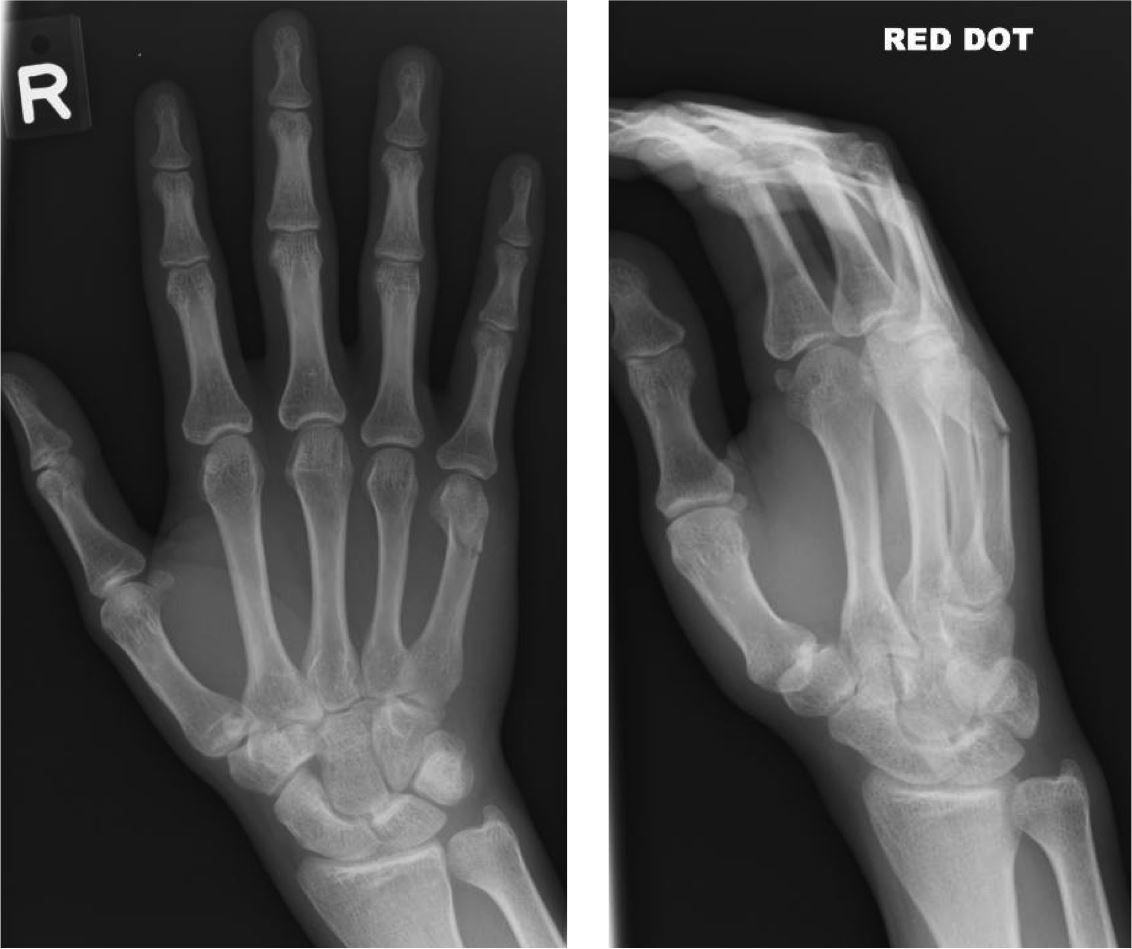
Long-term results have shown that persistent subluxation of the first carpometacarpal joint can result in marked degenerative changes and poor function. A metacarpal fracture affects one or more of the five metacarpal bones that run from the wrist ( carpal ) bones to the knuckles. However, close follow-up with frequent radiographs is necessary as redislocation and fracture redisplacement are common after conservative treatment. If anatomic reduction is obtained, a nonoperative course may be pursued. As the plaster dries, traction is placed on the thumb to pull the metacarpal distally with concurrent pressure pushing the metacarpal base ulnarly and volarly to return it to anatomical position. Closed reduction of a Bennett fracture can be attempted by applying a wet plaster thumb spica dressing. Whether a Bennett fracture should be treated by open or closed reduction is still a subject of discussion. This fragment is tethered by the uninjured anterior oblique ligament, while the main portion of the thumb metacarpal displaces radially, proximally, and dorsally by the pull of the abductor pollicis longus and the adductor pollicis. The fracture line has a typical oblique course creating a small triangular fragment on the volar-ulnar aspect of the metacarpal base. The injury occurs when the thumb metacarpal is axially loaded and partially flexed. This fracture was initially described by Bennett in 1882. The radiograph shown earlier illustrates a Bennett fracture. The intra-articular fractures can be further subdivided into Bennett and Rolando fractures. Fractures of the base of the thumb metacarpal can be divided into intra- and extra-articular fractures.
0 Comments
Read More
Leave a Reply. |
 RSS Feed
RSS Feed
